
“The Doc told me I have a herniated disc! Now What??” Budging or herniated discs are consistently some of the most feared diagnoses out there, especially in athletes. They see the MD for their back pain, get an x-ray or MRI, and they’re told one of the following. “Imaging is showing disc desiccation, disc prolapse, disc protrusion, disc fissure, disc bulging, a herniated disc, degenerative disc disease, foraminal encroachment, nerve root compression (or impingement), or stenosis. At this point you’re as white as a piece of paper and picture the worst-case scenario. Medical background or not, those are some pretty terrible descriptions of a picture taken of your spine. But here’s the truth behind it: 99% of the time, you’re going to be just fine. Stick with me as I dive into what the research says about your back and a bulging disc (Hint: surgery is not typically the answer).
Let’s kick this off talking about imaging, aka x-rays, MRIs, and CT scans. Imaging is a powerful tool to show providers a glimpse of what’s going on internally within the body. MRI’s in particular can show incredible detail relating towards inflamed or degenerated tissue. Oftentimes, imaging shows us so much detail that we will have “abnormal” findings that may not even correlate to the symptoms. Therefore, without a thorough examination, just using the picture to diagnose a problem isn’t enough. We simply don’t know if the findings are related to the patients symptoms, OR, if they are just age-related changes…. like grey hair. Let me explain further. Take a look at the graphic below, which shows common findings from images of the spine in individuals with NO BACK PAIN AT ALL!

There are 2 massive takeaways here:
1) Look at the 30’s group. 50% of people in this group showed disk degeneration and 40% showed a disc bulge. 50%! These numbers are HUGE. I sure didn’t think about bulging discs in my back at 30, and most people would consider this very rare for a 30 something year old to have a pain from a bulging disc.
2) The number of “positive” findings exponentially increases in each age group. So, the older you are when you start to experience any sort of back pain, the higher the chance you would show positive findings in the event you get an MRI or CT scan. This is why face-to-face examinations are SO important – they can help to delineate whether or not your back pain is truly from a disc issue, or something totally different (joints, muscles, etc.)
So, what signs and symptoms would you have that indicate a herniated disc? Let’s discuss. First things first, because of how close the disc sits in proximity to the nerve, we are always looking out for some major red flags regarding this anatomical relationship. Two red flags that require immediate physician attention are the loss of the ability to walk, or the loss of control over your bowel and bladder. These indicate that the spinal cord itself is being compressed. No bueno. Let me repeat, if you’re having these symptoms it is an emergency and please call 911 to safely get to the Emergency Room rather than reach out to us!
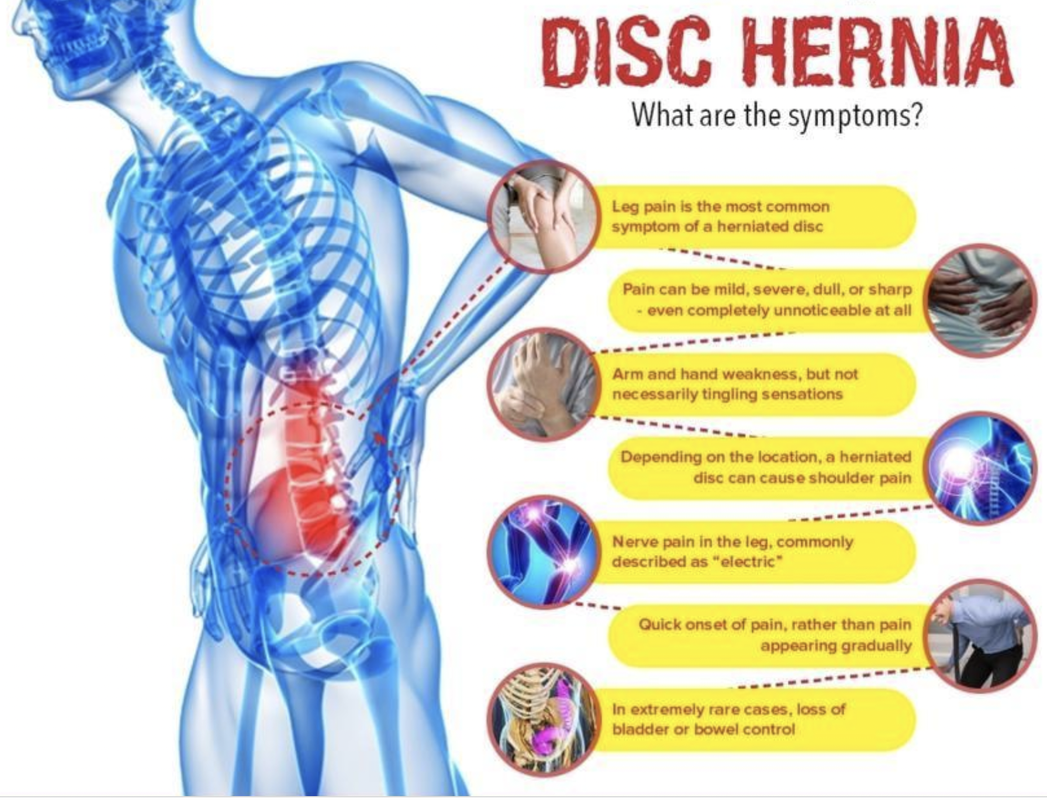
Other more common symptoms of a herniated disc, that are less severe and not a medical emergency, include nerve pain down one or both legs (that may include numbness and tingling or weakness), significant muscle weakness, loss of sensation on the skin, pain with unloaded flexion (lying on your back and bringing both knees to chest increases pain), increased pain with coughing or sneezing, pain significantly worse in the morning, and pain worsened by repeated bending forward. If you don’t have ALL of these lesser symptoms, your pain is most likely related to something other than herniated disc….. Let that sink in. That’s a decent sized collection of specific symptoms that must ALL be present. Considering this, the reality is that a true disc herniation being the cause of your pain is actually pretty rare.
So, the doc has diagnosed you with a herniated or bulging disc, and what are your next steps? Let’s start here with a statement from the American Academy of Neurological Surgeons:
“The initial treatment for a herniated disc is usually conservative and nonsurgical. A doctor may advise the patient to maintain a low, painless activity level for a few days to several weeks. This helps the spinal nerve inflammation to decrease. Bedrest is not recommended. The doctor may recommend physical therapy. The therapist will perform an in-depth evaluation, which, combined with the doctor’s diagnosis, dictates a treatment specifically designed for patients with herniated discs.”
If you go by what Dr. Google has to say about exercises to do, here’s what you’ll find:

Now, here’s what physical therapy SHOULD look like for your low back pain. During the initial evaluation we discuss the history of your low back pain including onset and what gives you relief or increases pain. We also begin to address other significant factors that play a role in the development of low back issues such as: sleeping positions, postures you spend all your time in at work, and workout history/current programming. Then, it’s time to get you up and moving. We look at how you move through a handful of different functional motions to get an idea of any areas with mobility and strength imbalances and restrictions contributing to your pain.
After that, we go through a more in depth assessment of each involved joint for mobility restrictions. In the presence of low back pain, we have to look at the Spine, SI Joint, Hips, Knees and Ankles as they all can play a role in having back pain while working out. From the collection of information we gathered regarding your injury to this point, we then educate you on where the pain is coming from, what we plan to do about it, and how to keep it coming back. This also includes discussing workouts and how to modify (Not just rest!) so that you can continue working out around the pain! After all the evaluation, the rest of the time remaining in the first visit is treatment to purely get you some pain relief and walking away from the clinic feeling better that day!
These are some common exercises we use after that first visit to start getting you moving again and getting the pain to calm down outside of the clinic. Notice, we keep the spine in a drastically different position than Dr. Google. The majority of time, with low back pain, moving into back extension such as the cobra pose only makes the pain much much worse!
So, we now know that full blown symptomatic disc herniations are actually pretty rare, that imaging will tend to show you some sort of disc related condition (even without back pain), and the first line of treatment is physical therapy. Unfortunately, not all physical therapy is the same. If you’ve seen a PT for low back pain in the past, here we do things quite a bit different. At The Charlotte Athlete, low back pain is the number one most common body region we treat, and the key to treatment in this region of the body is getting down to the root cause of why the pain occurs. Taking this approach, and addressing how you move, allows us to have excellent outcomes and even help some people who have had decades of low back issues. If this sounds like you, we would love to help. The next step is a free 20 minute phone call so we can learn more about your specific injury history and discuss how we can help!
Thanks For Reading!!
– Dr. Mike


3 Responses
Shouldnt people with herniated discs avoid flexion completely though? Even when the herniation has “healed”? Ive got a herniated disc extrusion (3 months in!) So I’m nervous looking at those excercises bc when I’ve “healed” that flexion might cause a reherniation
Hey Lauryn, just wanted to check in with you regarding your back – how is it? To answer your question, no, they should not avoid flexion completely. Whoever gave you this advice is not fully educated in how the body works unfortuntaely. Hope you are doing well!
An intriguing discussion is worth comment. I do think that you should publish more on this topic, it might not be a taboo subject but generally people dont speak about such subjects. To the next! Cheers!!